Introduction
The healthcare industry is undergoing one of the most profound transformations in its history, driven by rapid advances in artificial intelligence (AI). What began as experimental expert systems in research labs has evolved into a mature ecosystem of machine learning models, generative AI platforms, and intelligent devices embedded across the clinical value chain. From diagnosis and drug discovery to clinical documentation and hospital operations, AI is no longer a peripheral innovation; it is becoming a core capability for modern healthcare systems seeking higher quality, lower costs, and better patient experience.
For GenAI experts, the story of AI in healthcare is about the convergence of data maturity, compute scalability, regulatory evolution, and shifting clinician and patient expectations. At the same time, this narrative must remain accessible to non-technical readers, pairing technical terminology with clear explanations and using real-world market data to ground the discussion.
Historical Trajectory: From Expert Systems to Deep Learning
The Era of Expert Systems (1970s-1990s): AI in healthcare did not start with deep learning or large language models. Early work in the 1970s focused on rule-based "expert systems" designed to emulate human clinical reasoning. One of the most famous examples was MYCIN, developed at Stanford University to support the diagnosis and treatment of bacterial infections. MYCIN used a knowledge base of approximately 600 if-then rules and a reasoning engine that asked clinicians structured questions, then recommended antibiotic regimens adjusted for patient-specific variables such as weight and allergy status.
Remarkably for its time, MYCIN achieved performance comparable to, and sometimes better than, infectious disease experts in controlled evaluations. Despite its technical success, MYCIN never went into routine clinical deployment. The reasons are instructive: lack of integration with hospital workflows, limited computing infrastructure, and concerns about accountability if an AI recommendation led to harm.
The Deep Learning Revolution (2012-Present)
The current wave of AI in healthcare is largely a consequence of three forces maturing in parallel:
- Data digitization: Electronic health records (EHRs), connected devices, and the completion of the Human Genome Project created unprecedented volumes of structured and unstructured data
- Computing power: Advances in GPU technology and cloud infrastructure enabled processing of massive datasets
- Algorithmic breakthroughs: Deep learning enabled models to learn complex patterns directly from raw data, rather than relying on manually encoded rules
A pivotal moment came in 2012 when AlexNet, a deep convolutional neural network, dramatically outperformed traditional computer vision techniques in the ImageNet competition. While this benchmark came from the general computer vision community, its impact on healthcare was immediate: similar architectures were quickly adapted to interpret radiology images, pathology slides, dermatology photos, and ophthalmology scans.
This shift from rule-based expert systems to data-driven learning systems marks the key inflection point in the history of AI in medicine, enabling applications that can achieve diagnostic accuracy rivaling or exceeding human experts in specific domains.
Market Dynamics and Growth Outlook
Global Market Size and Projections
From a market perspective, AI in healthcare has transitioned from a niche segment to a high-growth strategic category. The global AI in healthcare market was valued at approximately USD 27-29 billion in 2024 and has already crossed the USD 37-40 billion mark by 2025.
Forecasts for 2032-2035 vary by methodology, but many converge on a potential market size in the range of USD 150-675 billion, implying compound annual growth rates (CAGR) typically between 36-44% range. This explosive growth reflects both technological maturation and accelerating clinical adoption.
Regional Distribution
North America currently leads in both market share and maturity, accounting for approximately 45-54% of global adoption. This dominance is supported by advanced health systems, strong venture investment, and a comparatively clear regulatory environment for AI-enabled medical devices.
Europe follows with steady growth, particularly in markets aligning national digital health infrastructure with AI innovation. However, Asia-Pacific stands out as the fastest-growing region at 42.5% CAGR, driven by large populations, rising middle classes, digital health leapfrogging, and government-backed AI initiatives.
India exemplifies this regional dynamism, with clinician AI adoption surging from 12% in 2024 to 41% in 2025?exceeding adoption rates in the U.S. (36%) and U.K. (34%). This rapid uptake is partly driven by the need to scale scarce specialist resources across large and diverse populations.
Technology and Component Segmentation
On the technology axis, machine learning (including deep learning) remains the dominant segment, accounting for approximately 40% of deployed AI solutions. Computer vision is the fastest-growing subsegment thanks to radiology, pathology, and ophthalmology use cases, with projected growth rates exceeding 20% CAGR.
Software platforms?ranging from decision support tools and imaging analysis systems to AI-powered clinical documentation products?represent the largest revenue component at 44-46% of the market. Services such as implementation, integration, and managed AI operations are growing quickly as health systems move beyond pilots to operational scale.
Return on Investment
AI implementations demonstrate compelling financial returns. Recent studies show that 79% of healthcare organizations currently utilize AI technology, achieving ROI within 14 months and generating $3.20 for every dollar invested. Among organizations deploying generative AI, 45% reported positive ROI within the first year.
Reported benefits include:
? Automation of 20-30% of administrative workload
? Reduction in coding and billing errors
? Lower readmission rates by 15-20%
? Average annual savings of $50,000-75,000 from administrative automation
? Improved patient retention rates by 15-25% through AI-powered engagement platforms
Core Application Domains Across the Care Continuum
1. Medical Imaging and Diagnostics
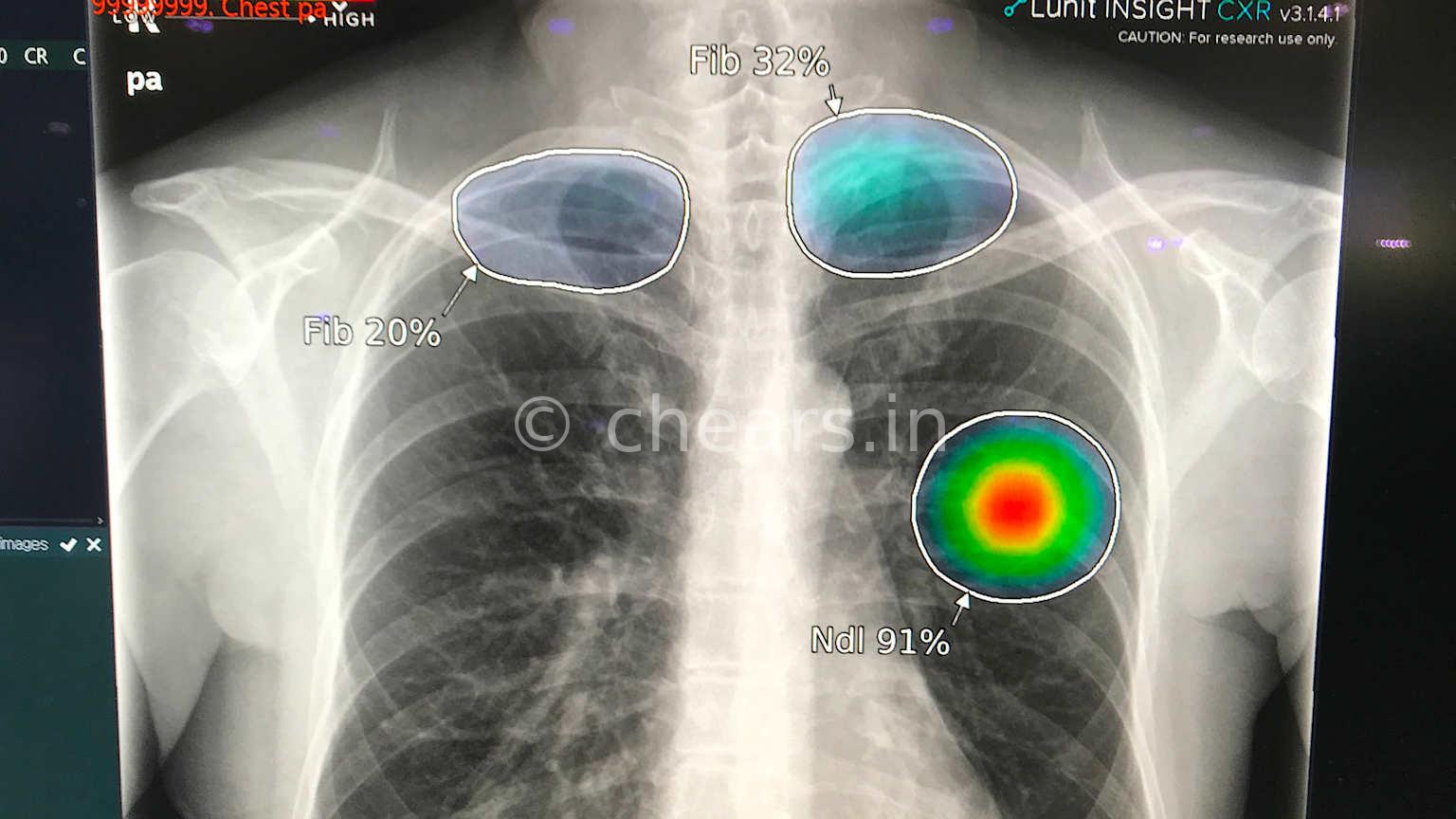
Medical imaging is the most mature and commercially advanced AI use case in healthcare. Deep learning models are now routinely used to support radiologists and other imaging specialists in detecting anomalies in X-rays, CT scans, MRI, ultrasound, and nuclear imaging.
Key Statistics:
- 75-80% of FDA-authorized AI/ML-enabled medical devices are for radiology
- As of mid-2025, the FDA had authorized over 1,200 AI devices since 1995
- 235 approvals in 2024 alone?the highest annual total in FDA history
- AI diagnostic accuracy exceeds 90% across multiple imaging specialties
AI algorithms have achieved high sensitivity and specificity in tasks such as lung nodule detection, breast cancer screening in mammography, intracranial hemorrhage detection, and retinal image analysis for diabetic retinopathy. The prevailing deployment pattern is "augmented intelligence" rather than fully autonomous AI: models serve as a second reader or triage tool, while final responsibility remains with the clinician.
2. Clinical Documentation and Ambient Intelligence
Generative AI and advanced natural language processing have opened a new front in clinical productivity: automated documentation. Ambient clinical intelligence systems passively "listen" to the clinician-patient conversation (with consent), transcribe it, and transform it into structured notes such as history of present illness, review of systems, assessment, and plan.
Impact on Healthcare Delivery:
- Shifts interaction from "eyes on screen" to "eyes on patient"
- Reduces documentation time per appointment by 30-50%
- Decreases after-hours "pajama time" for clinicians
- Improves clinician satisfaction and reduces burnout
- Achieves 100% engagement across responding health systems with 53% reporting high success rates
Platforms including Ambient Notes, AWS HealthScribe, and Abridge exemplify this category, utilizing sophisticated NLP models to generate structured documentation from conversational data. From a technical standpoint, these solutions combine automatic speech recognition, medical-domain large language models (LLMs), entity extraction for diagnoses and medications, and EHR-specific formatting logic.
3. Drug Discovery and Development
In life sciences, AI helps at multiple stages:
- Target identification: ML models mine scientific literature, omics datasets, and clinical data to identify novel biological targets
- Hit discovery and lead optimization: Generative models propose new molecules and estimate their binding affinity, toxicity, and pharmacokinetic properties
- Protein structure prediction: AI models infer 3D protein structures, enabling structure-based drug design
- Clinical trial optimization: AI improves patient cohort selection, predicts enrollment challenges, and simulates outcomes
Key Benefits:
- Reduction in discovery timelines by 30-50% for some phases
- Better probability of technical and regulatory success
- Platforms combining AI with quantum computing to identify promising candidates
- Faster responses to emerging health crises
4. Predictive Analytics and Personalized Medicine
Predictive analytics uses machine learning models to forecast future health events, such as risk of hospitalization, deterioration in chronic disease, or postoperative complications. These models analyze features from EHR data, lab values, prior admissions, medication adherence, and wearable device streams.
When combined with precision medicine, AI enables treatment personalization at scale. Precision medicine refers to tailoring treatments to the unique characteristics of each patient, including genomic profile, biomarkers, environment, and behavior.
Clinical Applications:
- In oncology: AI matches patients to targeted therapies and immunotherapies based on tumor genomics
- In cardiology/endocrinology: Models recommend individualized treatment intensities based on risk trajectories
- Population health management: Identifies high-risk cohorts early for proactive outreach
- Intensive care: Predicts hospital-acquired infections with 72% accuracy before symptom onset
Impact Metrics:
- Reduces hospital readmission rates by 15-20%
- Potential savings of billions in avoidable costs
- Enables value-based care models at scale
- Machine learning predicts urinary tract infections before symptoms in ICU settings
5. Telemedicine, Virtual Care, and Remote Monitoring
AI has transformed telemedicine from simple video visits into comprehensive virtual care ecosystems. AI-powered triage systems analyze patient symptoms to determine care urgency and recommend appropriate specialists?reducing avoidable ER usage.
Market Growth:
- AI in telemedicine market: $4.22 billion in 2024 ? projected $27.14 billion by 2030
- Represents a 36.4%CAGR
- Virtual health assistants provide 24/7 medical information in multiple languages
- Expands healthcare reach particularly in underserved areas
Remote Patient Monitoring (RPM):
Remote monitoring combines connected devices (blood pressure cuffs, glucometers, wearables) with AI models that detect patterns suggesting deterioration. For example, in heart failure, subtle trends in weight, heart rate, and activity can trigger early intervention.
As 5G and edge computing mature, near-real-time monitoring and closed-loop intervention (e.g., adjusting medications under protocol) become viable, enabling hospital-level care in patients' homes.
Technological Foundations Explained
Machine Learning (ML) and Deep Learning
Machine Learning is a field of AI where algorithms learn patterns from data to make predictions or decisions without being explicitly programmed. In healthcare, ML might learn from thousands of patient records to predict who is at highest risk of readmission.
Deep Learning is a subset of ML that uses multi-layered artificial neural networks to learn complex representations directly from raw data like images, waveforms, or text. Deep learning powers most state-of-the-art imaging and speech applications.
Key architectures:
- Convolutional Neural Networks (CNNs): Excel at image analysis for radiology, pathology, and dermatology
- Recurrent Neural Networks (RNNs): Process sequential data for patient monitoring and time-series analysis
- Transformers: Power modern NLP applications including clinical documentation
Natural Language Processing (NLP)
Natural Language Processing is the branch of AI that allows computers to understand, interpret, and generate human language. In healthcare, NLP reads free-text notes, extracts diagnoses and medications, and powers conversational agents and documentation tools.
Medical NLP capabilities:
- Named Entity Recognition (NER): Identifies medical terms like diseases, medications, procedures
- Clinical concept extraction: Links related data points (diagnoses with symptoms and treatments)
- Automated coding: Extracts relevant information for medical billing
- Report generation: Transforms imaging findings into structured radiology reports
Advanced models like BERT and domain-specific variants such as BioGPT, trained on biomedical literature, achieve unprecedented accuracy in clinical understanding and contextual interpretation.
Computer Vision
Computer Vision represents AI's capability to derive meaningful information from digital images and videos. In healthcare, this revolutionizes medical imaging interpretation.
Applications beyond diagnostics:
- Automated generation of structured radiology reports from scans
- Quantification of lesion size and tracking changes over time
- Quality control for imaging protocols
Conclusion
The advancement of artificial intelligence in the healthcare industry represents far more than incremental technological progress?it constitutes a fundamental reimagining of medical science and care delivery. From MYCIN's rule-based systems in the 1970s to contemporary deep learning architectures analyzing genomic sequences and predicting disease trajectories, AI has evolved from promising concept to indispensable clinical tool. Building trust requires transparency in algorithmic decision-making, rigorous bias mitigation, meaningful physician engagement in tool development, and regulatory frameworks balancing innovation with patient protection.
The imperative is clear: embrace AI not as replacement for clinical judgment but as augmentation of human expertise. For policymakers and regulators, the challenge involves crafting adaptive frameworks that encourage innovation while safeguarding public welfare. For technology developers, the responsibility extends beyond algorithmic performance to encompass ethical design, diverse representation, and seamless workflow integration.
The future of healthcare is not artificial?it is intelligently human, profoundly personalized, and powerfully preventive.